Diagnosis of pain from the sacroiliac joint
- Michele Curatolo

- May 22, 2023
- 4 min read
Updated: May 23, 2023

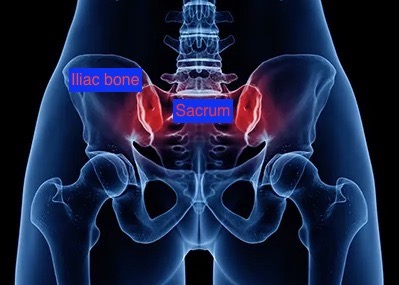
The sacroiliac joint connects the sacrum and the iliac bone, as shown in the picture below, and can be a source of low back pain. When examining patients, can we tell them whether the pain stems from the sacroiliac joint?
Traditionally, several tests of the clinical examination and imaging have been proposed, with limited evidence that such examinations rule in or out sacroiliac joint pain. Injections into the sacroiliac joint using local anesthetics can help identifying the joint as the source of pain: if patients experience substantial pain relief after injection of a local anesthetic, it may inferred that the pain likely stems from the sacroiliac joint. However, the test is invasive.
How can we evaluate the value of diagnostic tests for sacroiliac joint pain?
We want diagnostic tests to tell us whether a condition is highly likely or unlikely. We assume from literature data that 25% of patients with low back pain have pain from the sacroiliac joint (see here). Therefore, even before doing any test, a patient with low back pain has a probability of 25% and 75% to have sacroiliac joint pain or not, respectively. In order to be useful, a diagnostic test has to tell us that sacroiliac joint pain in a given patient is much more likely than 25% if the test is positive, and much less likely than 25% if the test is negative.
Most recent data on clinical criteria for sacroiliac joint pain
A recent systematic review pooled the results of different studies and identified two clinical criteria that contribute to the diagnosis of sacroiliac joint pain: absence of pain in the midline, and provocation tests. Based on these criteria, how confident are we to tell patients whether their pain originates from the sacroiliac joint or not?
The study used likelihood ratios to evaluate the performance of the tests. These numbers are difficult to interpret for patients and clinicians, and I will therefore convert them into probability or having or not sacroiliac joint pain (see here for the calculation and table below for a summary of findings).
1. Absence of pain in the midline
Absence of pain in the midline had a positive likelihood ratio of 2.44. This means that if the probability of having sacroiliac joint pain is 25% without collecting any history or doing any test, absence of midline pain increases the chance of having sacroiliac joint pain to 45%.
If this criterion is negative (i.e., the patient has pain in the midline), the negative likelihood ratio is 0.31. This means that the probability of having sacroiliac joint pain drops from 25% (if we do not consider pain location) to 9% in those patients with midline pain.
2. Sacroiliac joint provocation tests
According to the systematic review, another way to diagnose sacroiliac joint pain is to combine three or more provocation tests, which consist in applying maneuvers to the joint and try to elicit the patient's pain. Noticeably, the review found single provocation tests to be unhelpful, whereas the combination of at least three yielded a positive likelihood ratio of 2.44. This translated in a probability of having sacroiliac joint pain of 45%.
Absence of three positive provocation tests was associated with a negative likelihood ratio of 0.35, yielding a probability of having sacroiliac joint pain of 10% in those patients with less than three positive provocation tests.
What about imaging?
Bone scan consists in taking imaging after injection of a radioactive material that can be visible in the sacroiliac joint in case of putative pathology. When positive, bone scan had an excellent positive likelihood ratio of 7.33, which means a probability of sacroiliac joint pain of 71%. This is substantially higher than what we could expect without doing the scan (25%). However, a negative bone scan had a negative likelihood ratio of 0.74, implying a probability of sacroiliac joint pain of 20%. This is only insignificantly different from the 25% chance of having sacroiliac joint pain.
Summary of probability to have sacroiliac joint pain based on tests
The table shows the probability of having sacroiliac joint pain based on the results of the systematic review. The probabilities are calculated from the likelihood ratios provided by the study, assuming a prevalence of sacroiliac joint pain of 25% in patients with low back pain.
| | Probability of having sacroiliac joint pain |
Pain in the midline | Yes | 9% |
| No | 45% |
Three or more positive provocation tests | Yes | 45% |
| No | 10% |
Bone scan positive | Yes | 71% |
| No | 20% |
A caveat applies. All these studies have used injections of local anesthetics into the sacroiliac joint to evaluate whether the tests mentioned in the table are valid or not. The ligaments on the surface of the sacroiliac joint are also very pain-sensitive, and an injection into the joint do not anesthetize the ligaments. It is possible that pain at the sacroiliac joints stems, at least in part, from those ligaments and not from within the joint. To my knowledge, the value of the above tests for the diagnosis of pain from the sacroiliac ligaments has not been rigorously evaluated.
Conclusion
Some of the tests discussed above have limited value, as they do not change much the probability to have pain from the sacroiliac joint, as compared to an assumed probability of 25% for any patient with low back pain. However, the following findings can provide good support to the diagnostic process.
Pain in the midline is associated with a very low chance of having sacroiliac joint pain (9%).
If less than three provocation tests are negative, the chance of sacroiliac joint pain is only 10%.
A positive bone scan is very informative, as it is associated with a probability of sacroiliac joint pain of 71%, much higher than the pre-test probability of 25%. However, the meaningfulness of ordering a bone scan is questionable, as a negative finding would not be informative.